Advanced Health’s Prior Authorization Data
To comply with the CMS Interoperability and Prior Authorization final rule, Advanced Health is required to annually report aggregated prior authorization metrics on our website. Specifically, this includes a list of all medical items and services (excluding drugs) that require prior authorization, as well as data on prior authorization requests for those items and services (e.g., approvals, denials, etc.) over the previous calendar year. Publicly reporting these metrics promotes transparency and accountability, helps patients understand prior authorization processes, and enables providers to evaluate payer performance. In addition, metrics can be used to compare plans, programs, and payers.
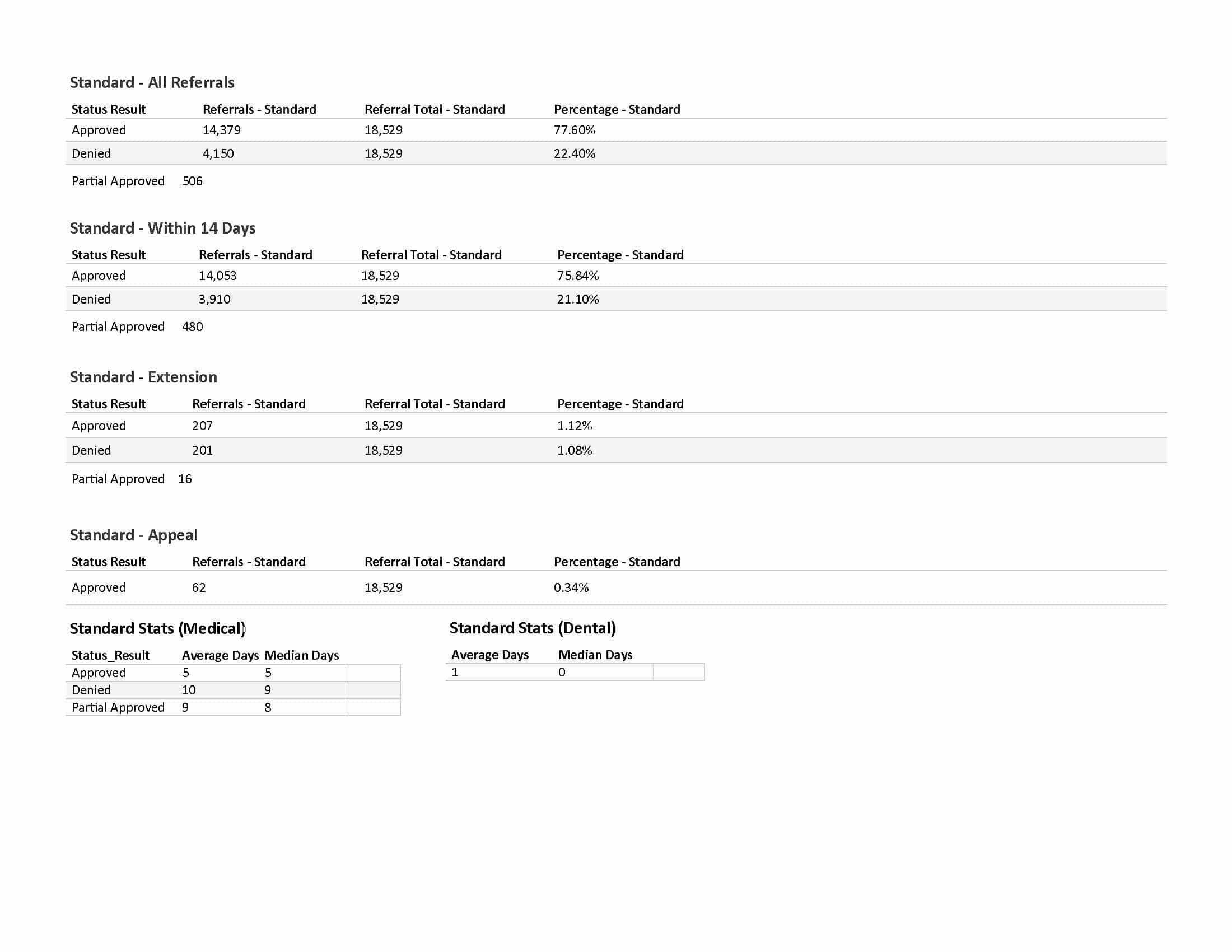
In 2025, Advanced Health received a total of 18,529 standard (non-urgent) prior authorizations for our covered patients. 77.60% of those requests were approved:
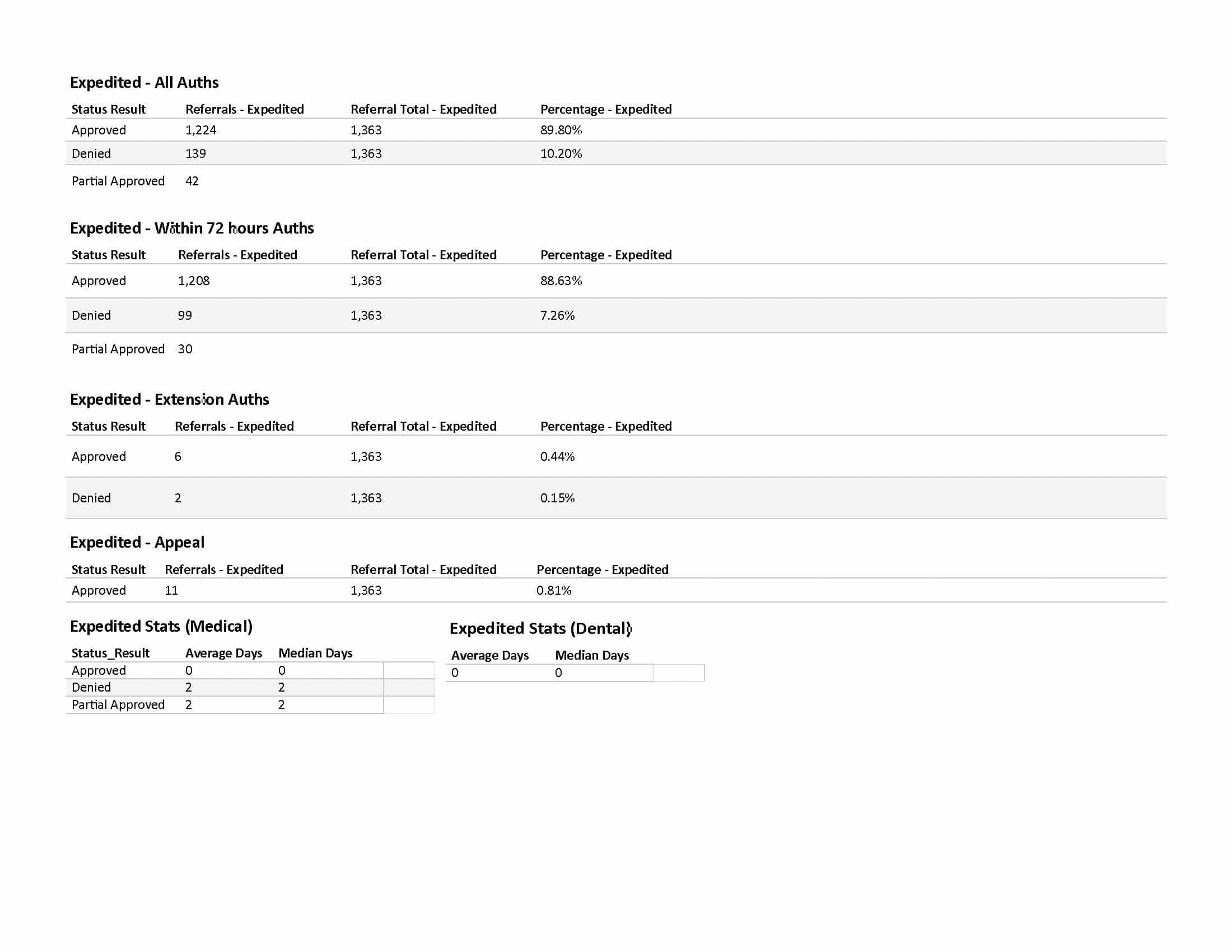
In 2025, we received a total of 1,363 expedited (urgent) prior authorization requests for our covered patients. 89.80% of those requests were approved: